It seems we can’t find what you’re looking for. Perhaps searching can help.
Page not found (404)
Recent Articles
-

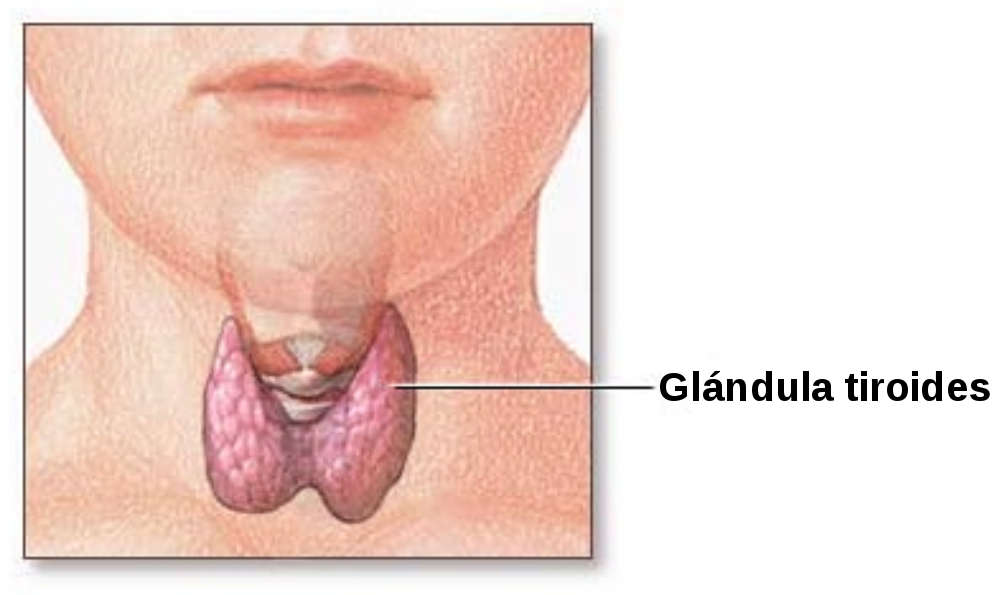
CBD Oil and Thyroid Medication
April 14, 2020 0 -
 April 7, 2020 0
April 7, 2020 0 -
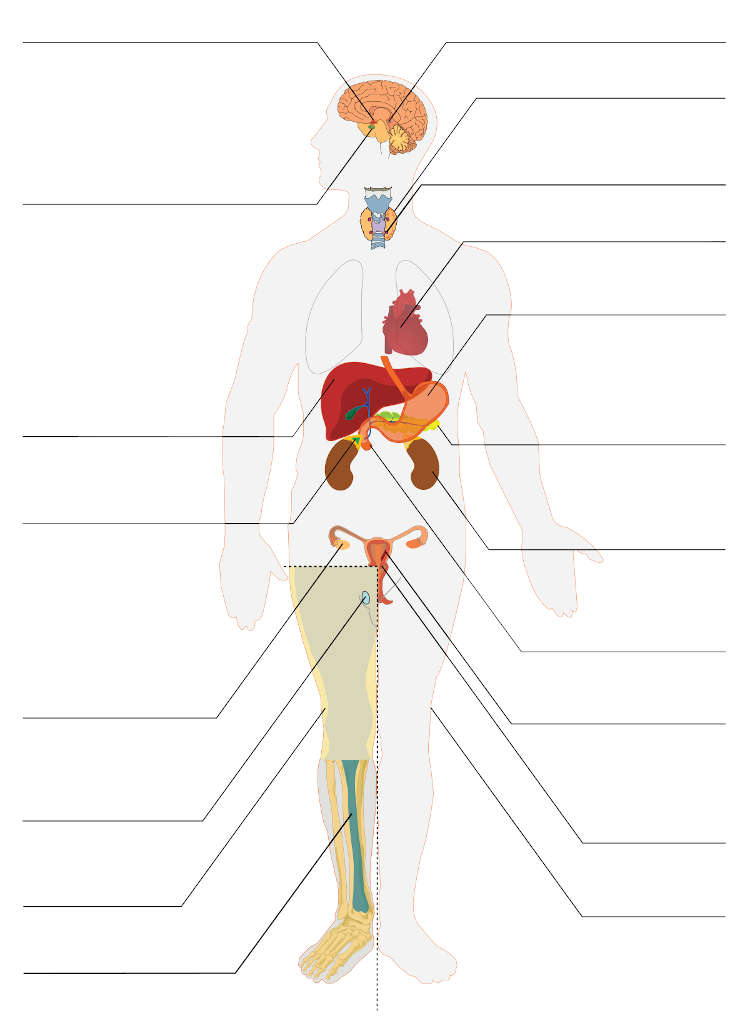
The Effects of Cannabinoids on the Endocrine System
April 5, 2020 0 -
 April 5, 2020 0
April 5, 2020 0 -
 April 5, 2020 0
April 5, 2020 0